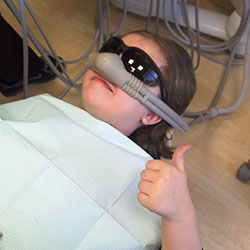
Sedation Dentistry
Sedation dentistry refers to the use of sedation during dental treatment. Sedation is most commonly used during extensive procedures, for patients with dental phobia or for patients who find it difficult to sit still. There are different types of sedation, including nitrous oxide ("happy air"), oral sedatives and general anesthetic.
Sedation can range from the use of nitrous oxide to calm a patient to general anesthetics used to put patients to sleep. Patients with dental phobia, low pain tolerance, major dental treatment, physical handicaps or strong gag reflexes may require sedation. Procedures like fillings, crowns, bridges, root canals, extractions, cosmetic procedures and periodontal treatments often require sedation.
Sedation is endorsed by the American Dental Association and is an effective way to make many patients comfortable during their dental visit. Before using a sedative or anesthetic, it is important to tell your pediatric dentist about any medications or medical treatments your child is receiving. Before administering any sedative or anesthetic, your pediatric dentist will talk to you about the process of sedation and pre- and post-sedation instructions.
Nitrous Oxide
Nitrous oxide, we use the term "happy air", is often used as a conscious sedative during a dental visit. The gas is administered with a mixture of oxygen and has a calming effect that helps phobic or anxious patients relax during their dental treatment. Because it is a mild sedative, patients are still conscious and can talk to their pediatric dentist during their visit. After treatment, the nitrous is turned off and oxygen is administered for five to 10 minutes to help flush any remaining gas. The effects wear off almost immediately. Nitrous oxide rarely has side effects, although some patients may experience minor nausea and constipation. Your pediatric dentist will provide you with pre- and post-sedation instructions.
Dental Surgery
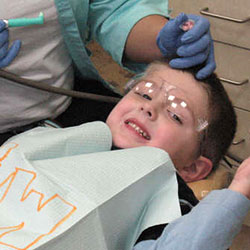 No doubt about it, getting an operation can be stressful for kids and adults alike. If your child is scheduled for surgery, you may have questions or concerns about anesthesia, in particular. The thought of your child being unconscious or temporarily losing sensation can be downright unnerving, whether your little one is 7 months or 17 years old.
No doubt about it, getting an operation can be stressful for kids and adults alike. If your child is scheduled for surgery, you may have questions or concerns about anesthesia, in particular. The thought of your child being unconscious or temporarily losing sensation can be downright unnerving, whether your little one is 7 months or 17 years old.
From a minor routine dental procedure to a more serious surgery in which your child will be "deeply sedated," knowing the basics about anesthesia may help answer your questions and ease some concerns — both yours and your child's.
About Anesthesia
Basically, anesthesia is the use of medicine to prevent the feeling of pain or sensation during surgery or other procedures that might be painful (such as getting stitches or having a wart removed). Given as an injection or through inhaled gases or vapors, different types of anesthesia affect the nervous system in various ways by blocking nerve impulses and, therefore, pain.
Our highly trained professionals use a wide variety of safe, modern medications and extremely capable monitoring technology. An anesthesiologist is a doctor who specializes in giving and managing anesthetics — the medications that numb an area of the body or help your child fall and stay asleep.
In addition to administering anesthesia medications before the surgery, the anesthesiologist will:
- monitor your child's major bodily functions (such as breathing, heart rate and rhythm, body temperature, blood pressure, and blood oxygen levels) during surgery
- address any problems that might arise during surgery
- manage any pain your child may have after surgery
- keep your child as comfortable as possible before, during, and after surgery
Parents' Concerns
When your child is having any kind of procedure or dental surgery, it's understandable to be a little uneasy. You probably have plenty of questions about everything — from how the anesthesia is given, to what your child will experience, to where you're allowed to be.
What happens will, of course, depend on the type of procedure your child is getting and the kind of anesthesia that will be used, either:
- general — in which your child would be "deeply sedated"
- local — when one small part of the body is numbed
To ease your mind and feel more informed, here's a quick look at what may happen before, during, and after on the day of your child's procedure in our office, just as it is in the hospital setting.
Although you may be able to talk to the anesthesiologist a day or two prior to the operation, you may not meet until that day. Either way, the anesthesiologist will go over your child's medical history and information thoroughly, so that he or she can give the right amount of anesthetic medications tailored specifically to your child's individual needs.
The anesthesiologist may also order additional tests (such as X-rays, blood or laboratory tests) to help figure out the best possible personalized anesthetic plan for your child.
In addition to doing a physical examination of your child's airways, heart, and lungs, the anesthesiologist will also want to go over your child's medical history, which will include asking about:
- your child's current and past health
- your family's health
- any medications, supplements, or herbal remedies your child is taking (consider bringing a list of exactly what your child takes, detailing how much and how often)
- any previous reactions your child or any blood relative has had to anesthesia
- any allergies (especially to foods, medications, or latex) your child may have
- whether your child smokes, drinks alcohol, or takes recreational drugs (this usually applies to older teenagers)
The anesthesiologist and/or Dr. Gunsaulis will also let you know whether your child can eat or drink before surgery. It's important to make sure that your child doesn't eat anything prior to surgery (usually nothing after midnight the day before the operation). You'll get specific instructions based on your child's age, medical condition, and the time of day of the procedure.
Why is eating before surgery an issue? The body normally has reflexes that prevent food from being aspirated (or inhaled) into the lungs when it's swallowed or regurgitated (thrown up). Anesthetic medications can suspend these reflexes, which could cause food to become inhaled into the lungs if there is vomiting or regurgitation under anesthesia. Sometimes, though, the anesthesiologist will say it's OK to drink clear liquids or take specific medications a few hours before surgery.
To ensure your child's safety during the surgery, it's extremely important to answer all of the anesthesiologist's questions as honestly and thoroughly as possible. Things that may seem harmless could interact with or affect the anesthesia and how your child reacts to it.
General Anesthesia
The goal of general anesthesia is to make and keep a young dental patient completely unconscious, deeply sedated, during the operation, with no awareness or memory of the surgery. General anesthesia is started by inhaling gases by breathing into a mask and after the child is unconscious, general anesthesia can be given through an IV (which requires a needle stick into a vein, usually in the arm). In our office we like parents to escort their child to our treatment room and remain until your child is deeply sedated. In the hospital, parents are not allowed in the operating room.
If your child is having general anesthesia, the anesthesiologist will be there before, during, and after the operation to monitor the anesthetic medications and ensure your child is constantly receiving the right dose. With general anesthesia, the anesthesiologist uses a combination of various medications to:
- relieve anxiety
- keep your child asleep
- minimize pain during surgery and relieve pain afterward (using drugs called analgesics)
- relax the muscles, which helps to keep your child still
- block out the memory of the surgery
After surgery, the anesthesiologist reverses the anesthesia process to help your child "wake up." It usually takes about 45 minutes to an hour for children to recover completely from general anesthesia. This recovery period is monitored by specially trained nurses either in the post-anesthesia care unit of the hospital or the recovery room in-office. During recovery, your child is still under the care of the anesthesiologist.